Five elements to set up a successful diabetes clinic
Two leading private diabetes care institutions in Africa met virtually to share their stories and discuss multidisciplinary diabetes care models across the continent: the Lions Diabetes Care Centre of MP Shah Hospital in Nairobi, Kenya and the Centre for Diabetes and Endocrinology (CDE) in Johannesburg, South Africa. Some fifty-eight healthcare professionals, medical and pharmaceutical business executives joined in the live discussion on 4th June. Their objective? To identify the key elements that a private healthcare provider should consider before establishing a diabetes clinic. This event was part of Diabetes Africa’s ‘Active Conversations’ series, examining diabetes care in a changing world.

Key points
- A multidisciplinary care model can deliver better outcomes for patients and remain affordable, particularly for middle-income patients in Africa;
- Proper medical upskilling of healthcare professionals is necessary, but not sufficient: professionals need to be taught how to operate effectively as a team, whether they are co-located or remote. External partners and funders need to understand the value of the services provided;
- To be sustainable, the clinics can rely on partnerships with private insurers (CDE) or tailored consultation packages paid directly by the patient (MP Shah Hospital). Communications and marketing are important, particularly in areas where such services are new;
- A multidisciplinary diabetes team can include, but is not limited to: a diabetologist or endocrinologist, registered nurses, a pharmacist, a diabetes educator, a dietitian, a podiatrist, an eye specialist, and a psychologist. All team members should have specialised training in diabetes care;
- A dedicated project leader with a persistent approach and good knowledge of diabetes care is instrumental in getting such a clinic off the ground.
The question
Video 1 Why establish a diabetes clinic? Dr Toseef Din, CEO of MP Shah Hospital gives an overview of the hospital’s Diabetes Care Centre.
1. Design a method of integrating diabetes care
Nairobi’s MP Shah Hospital established its first Diabetes Care Centre in 2017, with the support of the Lions Club International. It has since used the model to create additional clinics that serve different neighbourhoods in the capital city of Kenya. Arv Kalsi, the strategic consultant and architect of the programme refers to them as “one-stop care centres”.
The Centre for Diabetes and Endocrinology, based in Johannesburg, was founded in 1994 by Dr Larry Distiller. He describes the original CDE clinic, still in operation today, as a “medical home, where clients can come and get everything in one place”. Two other CDE-affiliated centres operate along the same model. In addition, some 165 CDE-certified general practitioners and endocrinologists provide the same services in a decentralized manner across South Africa.
The common thread between these clinics is to provide integrated care, delivered by multidisciplinary teams.
For Diabetes UK “Integrated care is about designing a system that focuses on the patient’s perspective of care. The delivery of integrated care is facilitated by integration of processes, methods and tools, which enable patients to move between services according to need.” These facilities deliver integrated diabetes care by linking seamlessly primary, community and specialist care. This integrated approach is likely to reduce the cost of treating diabetes by mutualising operational costs among healthcare professionals and reducing the risks of complication, as patient education and specialist care are part of the patient journey from the beginning.
In Africa, integrated care can be a pathway to accessing a broader range of healthcare professionals and services.
In Africa, integrated care can be a pathway to accessing a broader range of healthcare professionals and services. “Our socialisation is not towards preventative healthcare” Michael Brown, Diabetes Care and Education Specialist at CDE, observes. “Most of us are socialised to think that when we’re sick, we go and see the doctor.” Consequently, “a number of people are not prepared to pay for educators, dieticians and podiatry services, but are quite happy to see these people when it’s part of a managed programme.”
Another element common to these models is the use of multidisciplinary teams, who have been shown to deliver superior outcomes when treating people with diabetes. This is because the complexity of cases and number of factors at play, particularly with Type-2 diabetes, call for a holistic approach to diabetes care. A look at the minimum care provided by CDE shows that at least seven types of healthcare professionals can work together to accompany people with diabetes: general practitioner or endocrinologist, nurse educator, dietitian, podiatrist, ophthalmologist, biokineticist and clinical psychologist (Table 1).
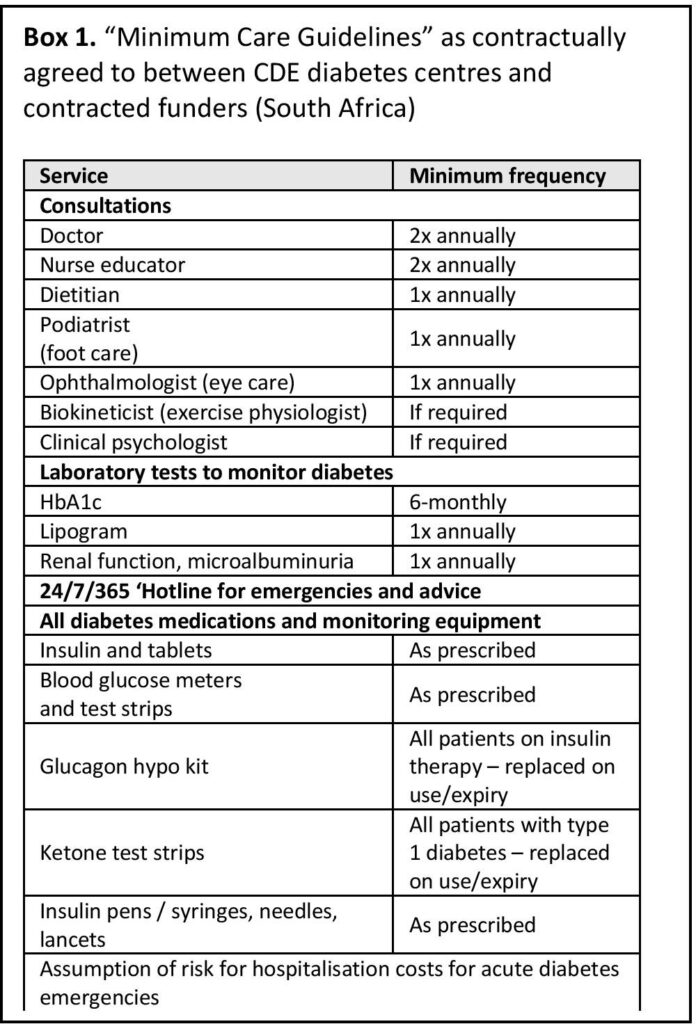
Table 1. “Minimum Care Guidelines” as contractually agreed to between CDE diabetes centres and contracted funders (South Africa)
*Replaced on use/expiry
However, Mr Brown is keen to point out that a multidisciplinary team is not just a group of healthcare professionals working in the same location. According to him, “what constitutes a team is a group of people who are specialised in their areas, but who work with each other, meet regularly and respect each other’s viewpoints.” “They’re also happy to collaborate across the grey areas at the intersections of their varying specialties of practice.”
The replay
Video 2 Michael Brown from the Centre for Diabetes and Endocrinology (CDE) in Johannesburg, South Africa, shares his views on what a multidisciplinary team is.
2. Select a sustainable funding model
To fund multidisciplinary diabetes care, CDE and MP Shah Hospital have adopted two different approaches. CDE has opted for a model by capitation, developed with medical aids, the main funders of private healthcare in South Africa, while MP Shah Hospital relies on direct payments from patients.
Dr Larry Distiller, Founder of CDE, explains that the initial financing model for the centre relied on insurance coverage for individual on a fee-for-service basis; this proved to be financially unsustainable. Key aspects of holistic diabetes care, such as podiatry, were insufficiently covered, putting patients at risks of complications and increasing the cost for the funders.
With the current model by capitation, health insurance companies pay the centre a fixed amount per patient per month, which is to cover all costs related to diabetes care: doctors’ visits as well as patient education, foot and eye care specialists, laboratory services and medication, including insulin. A basic minimum care package is agreed with the funders (Box 1).
“For that fee” Mr Brown explains “we take all the risks of managing diabetes day-by-day, including the management of acute emergencies such as hypoglycaemia and diabetic ketoacidosis”. As the overall cost per head is fixed, this creates an incentive for the centre to educate patients and reduce the risks of complications, which are often costly. Dr Distiller points out that this system reduces the cost of care for people with diabetes when compared to a segmented approach for care. It also provides adequate remuneration to key healthcare professionals, for example educators and dietitians.

At the heart of the MP Shah diabetes centre model is a differentiated offering that adapts to the patients’ needs and resources. Ms Kalsi explains that designing the care packages relied on extensive market research, to maintain a balance between optimal, affordable care and financial sustainability for the centres. The care packages include consultation fees as well as basic or advanced tests, depending on where the patients are in their journey. They can test their HbA1C levels, cardiac and kidney functions (Table 2).
Through operational efficiency and a reduced profit margin, the Lions Diabetes Care Centre can provide integrated diabetes care at a lower cost than individual private consultancies in the same area. As an illustration, Ms Kalsi notes that a visit to a private endocrinologist in Nairobi costs up to three times as much as seeing the same consultant at the Diabetes Care Centre, without the benefits of integrated care: in the centre, patients receive free diabetes education and can be seen by a team of specialists if required.
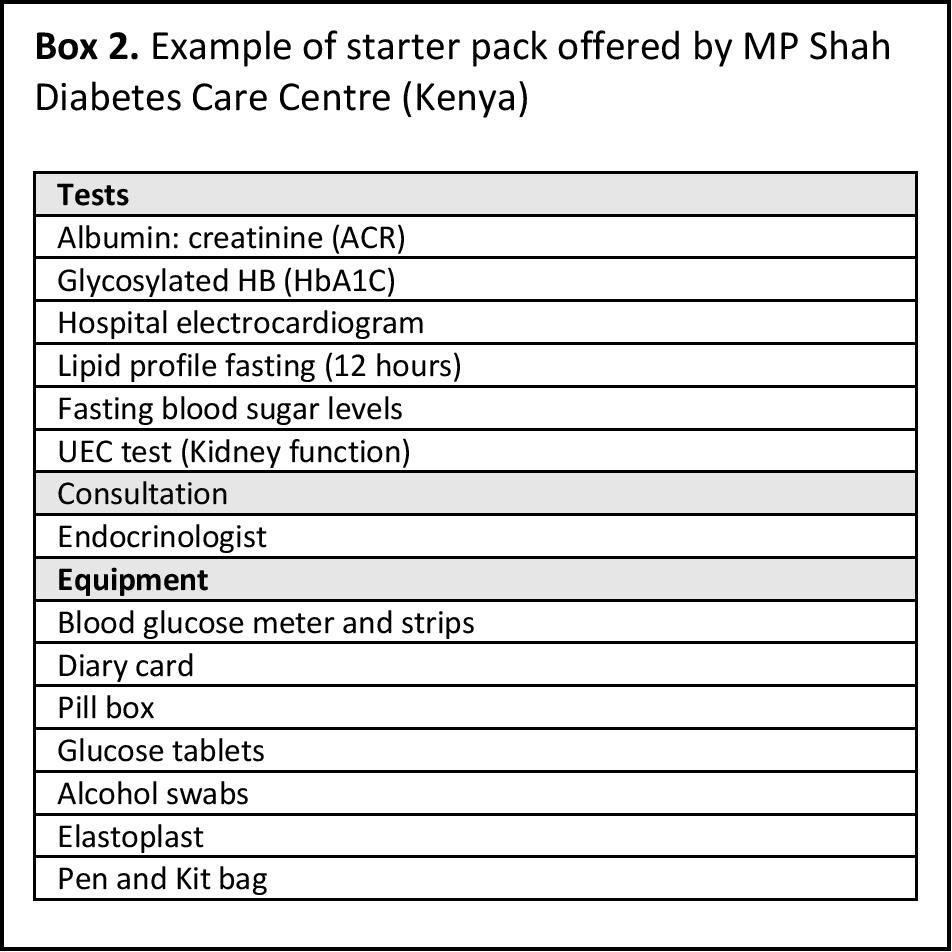
Table 2. Example of starter pack offered by MP Shah Diabetes Care Centre (Kenya)
3. Ensure adequate space and staffing for the clinic
Establishing a one-stop diabetes care centre or ‘medical home’ for people with diabetes begins with space, the amount of which depends on the extent of services that will need to be provided. “For the Diabetes Care Centre, we were given ample space by the MP Shah Hospital” Ms Kalsi explains. “This included: space for the reception, a triage room, consultancy rooms, and plenty of other rooms to host additional services: counselling, diabetes education, nutrition, examination and treatment.” The idea is to make the journey for the visitor as simple and comfortable as possible.
This philosophy extends to the induction of staff: “we developed guidelines because we wanted a standardised approach to guarantee good quality care for patients” Ms Kalsi, who supervised the six-week set-up of the MP Shah Hospital diabetes centre, explains. “From reception to the pharmacy to the consultants, everyone knows what the best practices are”. This induction can extend to the language used within the centre. “At CDE,” Mr Brown explains, “we prefer to use the word client, rather than patients when talking about the people who visit the centre. ‘Patient’ is associated with sickness and acute care. We look after healthy people and try to keep them well.”
Once the basis has been laid, the development of the centres can be modular, depending on the initial resources and space available. At the minimum, integrated care centre should provide access to a general practitioner trained on diabetes or an endocrinologist, a specialised nurse, a diabetes educator, a psychologist and a pharmacy.
The operational and communications functions are important as well. To support the development of the clinic, marketing staff need to be brought on board and understand the uniqueness of the multidisciplinary care offering.
4. Establish a training programme for the healthcare team
Dr Toseef Din, CEO of MP Shah Hospital highlights the importance of upskilling healthcare professionals on a continuous basis, despite the challenges. “In diabetes, many things keep changing and it is important for us to keep abreast of what is actually happening” She observes. The hospital has had to overcome obstacles and establish its own training programme for the Diabetes Care Centre: “in this part of Africa, training programmes are limited.” The centre is now in discussion to expand its learning programme to professionals working in the public sector.
The idea of sharing diabetes knowledge widely within the clinic is not only useful, it is indispensable: patients come in contact with a wide range of healthcare professionals in their journey and knowing when to refer to a specialist can save lives.
The CDE has been delivering diabetes training for professionals for more than twenty-five years. One of the drivers for the CDE training programmes was the necessity to provide a uniform standard of care across the centre’s network in South Africa; however, it has developed its reach across the continent, including in Kenya. For Dr. Saira Sokwalla, the consultant physician and diabetes specialist who now heads the MP Shah Diabetes Care Centre, “the teachings from CDE have been instrumental in our clinical management.”
People with diabetes come in contact with a wide range of healthcare professionals in their journey and knowing when to refer to a specialist can save lives.
5. Appoint a capable and resilient project leader
No diabetes clinic can take off without a passionate project leader. When asked about the steps required to deliver an integrated, multidisciplinary diabetes clinic, Dr Distiller answers candidly: “The first thing you need is a massive fire in your belly.” “It is difficult: you need to persuade private funders and the government of the advantages of multidisciplinary care.” And this expands to the people working around the project leader: “You’ve got to have a team around you that feels the same.”
Ms. Kalsi was the project leader for the Lions Diabetes Care Centre in Nairobi, and she continues to advise MP Shah Hospital on future expansions. In hindsight, she believes having a dedicated coordinator with good knowledge of diabetes and business development allowed the centre to be implemented in a record time of six weeks, an achievement that would have been difficult to deliver when relying only on medical staff without a business background.
In addition to passion, Ms Kalsi emphasizes the need for everyone involved to understand the objectives of the clinic and the local context. “The same model that we have in Kenya may not be suitable for yourself, because your target audience and market needs may be different.”
Future projects will be able to rely on a wealth of knowledge from CDE and MP Shah Hospital. Diabetes Africa has pledged to support the diabetes professional community in Africa.
Active Conversations examines diabetes care and health policy in a changing world. To stay informed of future events, join Diabetes Africa as a member or champion. For any queries about partnership please contact us.
Found this article helpful?

