Rethinking podiatry care in Africa
Healthcare professionals and business executives joined a spirited discussion last Thursday to tackle an ambitious topic: ‘Rethinking podiatry care in Africa’. Led by a podiatrist, an endocrinologist, and the head of the only academic podiatry department in Africa, the conversation addressed topics such as perceptions of the profession, multidisciplinary care and education. Over a hundred participants joined in the live discussion, which was part of Diabetes Africa’s ‘Active Conversations’ series, examining diabetes care in a changing world.

Key points
- All healthcare professionals should be aware of the risks of foot complications among people with diabetes, and refer to trained professionals as required;
- The COVID-19 pandemic has put a strain on patients with diabetes and foot complications: it preferable to do a foot examination in person;
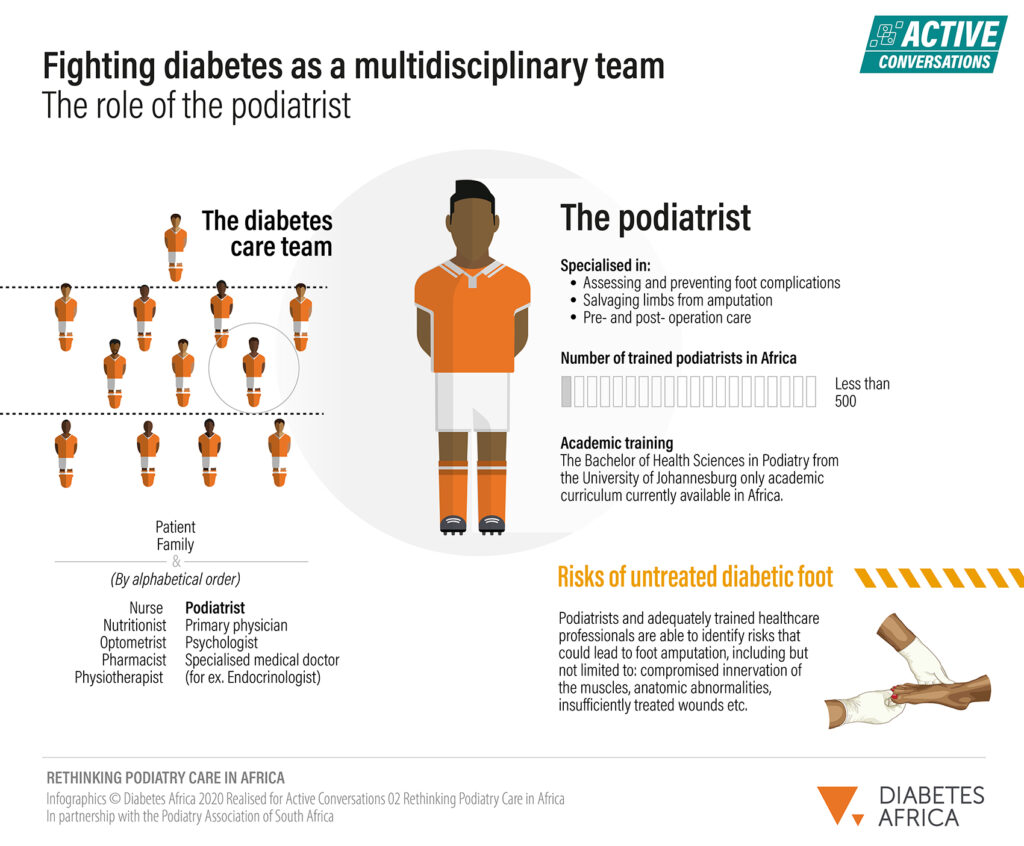
- There is currently only one formal academic curriculum for podiatrists in Africa, delivered by the University of Johannesburg;
- A multidisciplinary approach to diabetes care that includes podiatry can improve outcomes for patients. It should be encouraged during academic training, and incentivized at primary, secondary and tertiary care levels;
- Podiatrists can contribute to raising awareness about their role by collecting and disseminating data on their medical and economic impact, particularly with regard to diabetes.
The question
In picture
Facing COVID-19
The COVID-19 pandemic provided an obvious starting point for the conversation. The lockdowns and curfews established across Africa have forced healthcare professionals caring for diabetes patients to adopt new practices. Like other medical specialists across the continent, Dr Afokoghene Isiavwe, Endocrinologist at the Rainbow Specialist Medical Center in Lagos, has made greater use of telemedicine, using WhatsApp and Zoom calls to consult with patients. To provide basic foot care, she is guiding patients remotely and helping them look for signs of complications: “patients should check for any change in colour, and for any cracks, blisters or wounds”, she explained. “Some of them are able to use a 10g monofilament fiber to perform self-screening for loss of sensation.”
By and large however, specialist foot care professionals have found it difficult to adapt. “Before COVID-19, I had never managed patients without seeing them” Tshidi Mbonani, Senior Podiatrist and Chair of the Wound Care Committee at Chris Hani Baragwanath Hospital in Johannesburg, admitted. “Our job is mostly physical and requires us to be in contact with the patient, but we try and give advice as much as possible and we try and educate patients.” Participants in the conversation were quick to point out the limits of telemedicine and the ability of patients to self-diagnose. Simiso Ntuli, Head of the Podiatry Department at the University of Johannesburg and practicing podiatrist, described the harsh reality: “when you have a diabetic patient tell you ‘I think I have an ingrown nail’ and it is septic, there is very little you can do other than tell the patient ‘you need to come and see me.”
Educating patients and families
Many patients are not able to self-examine because of their age, weight or other conditions that prevent them from reaching and viewing the soles of their feet. Family members can provide basic support, but the extent of help that can be expected from them is debated. For Robert, a podiatrist and participant in the conversation, “patients are part of a community”, “training family members is a necessary exercise to improve outcomes.” Experienced podiatrists, such as Lucas Breedt, who is also the National Secretary of the Podiatry Association of South Africa, were more cautious: “some individuals can be heavy-handed and this may result in more harm being done than good” he observed.
In environments where footcare and podiatry are not widely available or well-understood, empowering patients and their families is important, but educators and specialists should be aware of the limitations. Ms. Mbonani explained her approach: “what I would usually do, whenever I have to teach a patient, is to have a family member there. That encourages continuation and understanding of care. But I also remind them of the potential risks and dangers.”
Treating patients at an early stage
People suffering from diabetic foot complications in Africa are often presenting late to a hospital or specialist. Saving a limb from amputation is not always possible, especially without a podiatrist involved. One way to avoid amputation is to make sure that diabetes patients know the risks of complications from the moment they are diagnosed. Dr Isiavwe was clear: “anybody who is living with diabetes, or any healthcare worker who is well-informed ought to know that foot ulcers in a person living with diabetes shouldn’t be taken lightly.”
The reasons for patients presenting late are multifaceted: low number of podiatrists, particularly in the public sector, lack of incentives, lack of understanding by other healthcare professionals of the role of podiatrists. For Ms. Mbonani, the psychosocial background is important: “we need to look at our patients’ thought processing of being diagnosed with diabetes and their understanding of that. Too often we hear patients say ‘I only have a little bit of diabetes’, thinking that they are not at risk of complications.”
For Mr Ntuli, there is a way to improve understanding of podiatry by other healthcare professionals, and eventually improve outcomes for patients: train healthcare professionals together. For him, the absence of a medical school at the University of Johannesburg, where South African podiatrists are trained, has been a disadvantage: “You’re finding that the medical schools will train physiotherapists, occupational therapists, and all sorts of healthcare practitioners, but podiatrists are trained away from those institutions.” According to him, the absence of podiatry in the medical university ecosystem “speaks to why other healthcare colleagues do not understand the podiatry profession.”

Simiso Ntuli
University of Johannesburg
“We need to learn to treat diabetes the way we play soccer: in a team. Not everyone needs to be a goalkeeper to ensure that the opposite team doesn’t score.”

Dr Afokoghene Isiavwe
Rainbow Specialist Medical Centre, Lagos
“Anybody living with diabetes, or any healthcare worker who is well-informed ought to know that foot ulcers in a person living with diabetes shouldn’t be taken lightly”

Tshidi Mbonani
Chris Hani Baragwanath Hospital
“Podiatry has evolved, the world has evolved and we need to evolve with it.”
Training healthcare workers
In countries where there isn’t yet a podiatry faculty, such as Nigeria, medical specialists have taken upon themselves to train healthcare workers, who are on the frontline of diabetes diagnosis and care, particularly in urban areas. Owen Bernard, President of the World Walk Foundation Jamaica Chapter explained the need to think outside-the-box and innovate: “There is currently a vacuum, and until the podiatrist arrives, we need to do what we can at the community level to prevent diabetes foot complications. This includes primary prevention, especially in resource poor settings in Africa.”
To fill the gap, Dr Isiavwe and her colleagues at the Rainbow Specialist Medical Centre in Lagos created a training programme on diabetes foot screening and foot care designed for primary care doctors, paramedics and nurses: the Diabetes Podiatry Initiative. Launched in 2014, the programme was subsequently expanded to other health care facilities in Lagos and the rest of the country with the help of the World Diabetes Foundation. Training faculty came from the Podiatry Institute of Georgia (USA) with Rahn Ravenell as the institute’s team lead.
Since 2018, Rainbow Specialist Medical Centre, in partnership with the World Walk Foundation Jamaica Chapter, also began a one-week Foot Care Assistant certification programme. The programme is targeted at primary health care workers and also offered to doctors and nurses.
Inspired in part by these initiatives, “several other foot care training missions have later sprung up in Nigeria, expanding foot care trainings beyond Lagos to other parts of Nigeria” described Dr Isiavwe. These programmes, developed by local and diaspora professionals as well as international organisations, include: the Mark Anumah Medical Missions, led by Prof Felicia Anumah of the University of Abuja, and the International Limb Salvage Foundation, led by James Fulwood.
As a direct result of these combined efforts, more trained nurses and paramedics are now able to carry out foot checks on persons living with diabetes. These checks can be carried out while patients await their appointment with doctors, for example.
Multidisciplinary care teams
For Mr Bernard Owen, “the objective is not to train everyone to become a podiatrist.” One of the objectives of training could be to teach healthcare professionals to refer patients to a more specialized professional when required. For Mr. Ntuli, this means that “we need to capacitate people correctly at the levels they’re at.”
This brought on the concept of multidisciplinary care. “We need to learn to treat diabetes the way we play soccer: in a team.” Mr. Ntuli explained. “Not everyone needs to be a goalkeeper to ensure that the opposite team doesn’t score.”
Adopting this approach means developing and promoting the concept of multidisciplinary care team. Dr. Isiavwe, who has adopted this approach with her own diabetes clinic in Lagos, agrees: “research has shown that multidisciplinary care teams can improve patient outcomes.”
However, the soccer team should still have at least one goal keeper: “we can understand that a physician might not feel confident and competent enough to approach foot complications”, Ms. Mbonani remarks. “This is why podiatrists have a role in the team.”

Moving forward
Observational data gathered in Africa has showed that early management of people with diabetes, with proper attention to foot care, can lead to a significant reduction of amputations. As a first-hand witness of this impact Dr Isiavwe called participants to “build on the momentum” and promote podiatry care across the continent.
Participants agreed that policies and training of healthcare professionals would benefit from a renewed approach of podiatry, but foot care specialists have role to play in providing structured evidence to inform decision-making. “We need to flood our governments with data”, Mr Ntuli suggested, explaining that “essential data on the socio-economic impact of diabetic complications” was missing. To produce this data, “podiatrists [will] need to work together” he added. There was certainly energy in the room to take on the task: “podiatry has evolved, the world has evolved and we need to evolve with it” concluded Ms. Mbonani.
Active Conversations examines diabetes care and health policy in a changing world. To stay informed of future events, join Diabetes Africa as a member or champion. For any queries about partnership please contact us.
Found this article helpful?

