Nigeria has less than 200 endocrinologists. Here is a way to bridge this gap.
In the wake of the disruption across sectors caused by the COVID-19 pandemic, there is an opportunity to use technology to improve on existing processes and better manage chronic diseases in Nigeria, especially for chronic diseases such as diabetes mellitus. Dr. Michael A. Olamoyegun from Ladoke Akintola University of Technology Teaching Hospital writes that telemedicine can play a vital role to help keep track of records and interact with patients without putting them at risk of catching the COVID-19 virus.

Missing accurate data in Nigeria
Diabetes is rampant in Nigeria, but accurate epidemiologic data is missing. According to research by Uloko et al[1], the current prevalence of diabetes mellitus is estimated at 5.77% and there is no systematic screening and recording of people with diabetes. Even with this conservative estimate, the task is daunting.
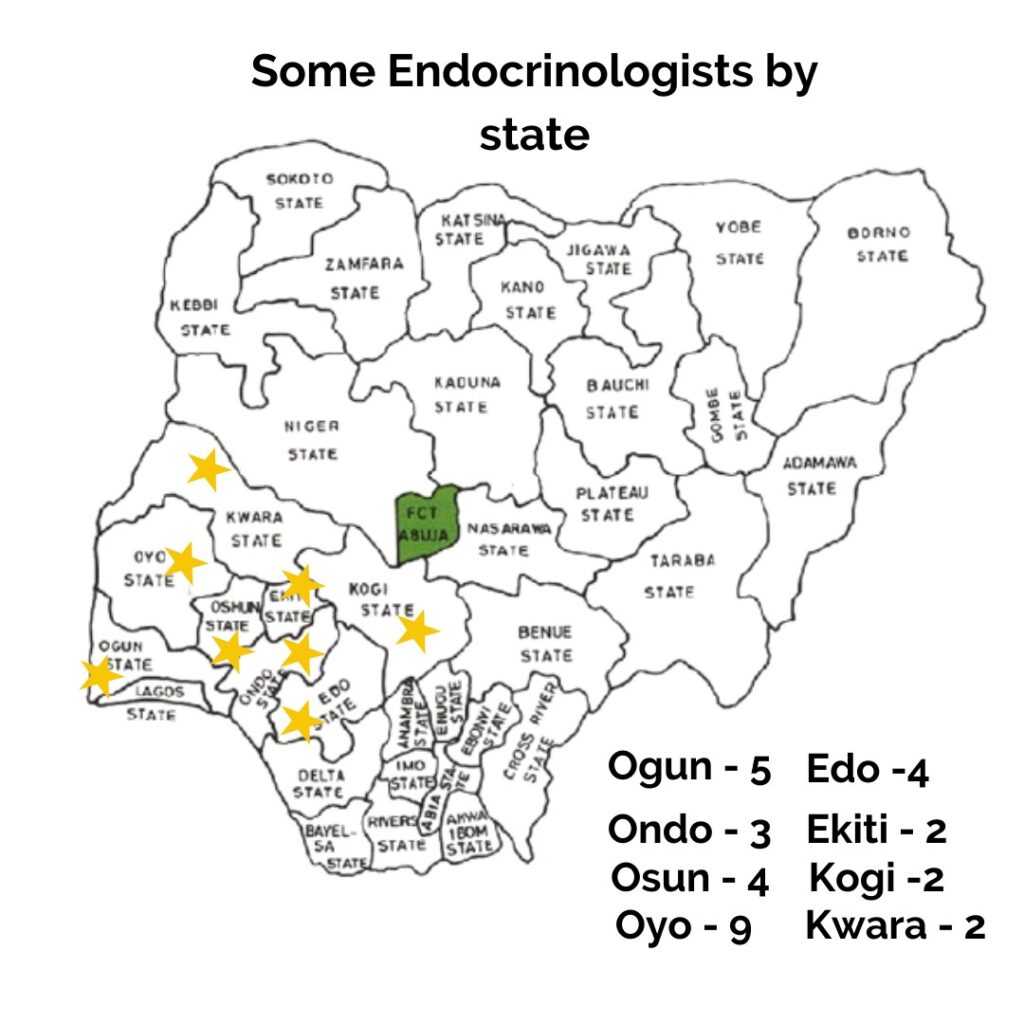
I am one of fewer than 200 endocrinologists in Nigeria. Using the rather conservative prevalence figure above, that’s one endocrinologist for 60,000 Nigerians living with diabetes.
Of course, other healthcare professionals can provide diabetes education and care, provided they have received adequate training, but many challenges remain in addition to the lack of specialists: low public health spending, inadequate facilities, maldistribution of clinicians. Between scheduled check-ups, patients often still require medical advice and monitoring and this is almost impossible in rural areas.
Based on my own early experience of being a physician working remotely with patients in the oil and gas industry in Nigeria, and knowing the work that LAUTECH teaching hospital is currently conducting, I truly believe that technology and particularly telemedicine can bridge this gap by virtually connecting physicians to patients, thereby improving patient management.
Why Telemedicine plays a key role
Telemedicine is simply the delivery of health care services using communication technologies for the exchange of information used in the diagnosis, treatment and prevention of diseases. It is called health care delivery at a distance because it ensures that remoteness is not a barrier to healthcare. We can achieve this by connecting virtually medical practitioners in urban areas to patients in underserved or rural communities, and by also linking practitioners in rural areas with colleagues in urban areas that can assist in patient management.
With 198.9 million active GSM subscribers in Nigeria, the mobile phone plays an important role in diabetes management. As a result of their ubiquity (especially basic phones), affordability and versatility, mobile phones are vital for telemedicine consultations. During the pandemic, I have myself carried out consultations through text messages, video calls, email and WhatsApp. While not perfect, these consultations were often the only thread linking a patient to my practice and to reliable, professional advice.
Mobile applications like Vsee, Mend, Lemonaid, and Glucose Buddy available in all common app stores are useful in patient care and education. They are of great use in extending specialist care to our patients, for relaying investigations, for prescriptions renewal, monitoring of exercise and diet, providing reminders for medication and clinic appointments, and storage of electronic health records.
I see tremendous potential for telemonitoring to be used in diabetes management. Trackers installed in mobile applications are synchronized with equipment used in reading and monitoring patients’ blood glucose levels. This equipment tracks glucose profile diaries, blood pressure, and oxygen levels and can share this information with registered care providers. Examples of this equipment include smartwatches that monitor exercise, heart rate, blood pressure, calories and sleep patterns, smart blood pressure monitors, smart pulse oximeters, smart glucometers such as the Accu-Chek Instant Meter, and flash glucometers that use implants under the skin to monitor blood glucose level without requiring constant finger pricks. Versatile platforms like Applinic can also be used to monitor multiple disease conditions and consult with specialists. The best part is that these apps are approved by bodies like the American Diabetes Association, and their results are comparable with those obtained from traditional methods of patient care.
Telemedicine can also be used in Diabetes-related services such as the management of diabetes mellitus foot syndrome (DMFS). The “see it, snap it, and send it” model encourages our patients to use cameras on mobile phones to share pictures of any abnormal features on their feet with us and receive prompt advice. We also have foot temperature monitoring mats that record and compare feet temperature, and this can help us monitor for inflammation and also guide patient care.
We also have tele-ophthalmology which is useful in the treatment of diabetic retinopathy. Smartphones can be modified to function as cheaper and easier-to-use alternatives to traditional retinal screening cameras, and the results sent to specialists for interpretation and advice.
Smartphone applications
Another vital application of telemedicine is in the management of hyperglycaemic emergencies which are the most common cause of mortality in diabetic patients.
In this aspect, the LAUTECH eHealth Research Group, a partnership of physicians from the diabetes unit of the LAUTECH Teaching Hospital (LTH), Ogbomoso and members of the LAUTECH Faculty of Information and Communication Technology, is creating a smartphone application for early diabetes emergency intervention. The application hosts patients, next-of-kin and physicians, and uses GPS and cellular network technology to monitor patients remotely. If patients experience any sudden symptoms, such as those of hyper- or hypo-glycaemia, they can report it via the application, which then sends an emergency SMS with the patient location, time and clinical condition to their next-of-kin and managing physician. The incorporated GPS technology helps patients locate the nearest health centre for prompt care, and it also allows the attending physician access to patient health records in cases of an emergency.
The benefits of telemedicine are clear, and that is why at our diabetes mellitus clinic in LAUTECH Teaching Hospital, we use smartphones to create electronic health records for our patients. We also interact regularly with them using WhatsApp.

Photo. Members of the LAUTECH eHealth Research Group (Nigeria). From left to right: Dr Orugun; Dr Olamoyegun (Head of the Centre) & Dr Adeyemi.
Our clinic hopes to expand its use of telemedicine via a Diabetic Rural Outreach Project (DROP) that connects patients and local primary care providers in rural Oyo state communities with urban specialists’ centres for glycaemic management. Primary health care centres and general hospitals in the state can also be equipped with infrastructure to host patient data and liaise with tertiary centres like LAUTECH Teaching Hospital to provide virtual consultations. This development would be useful for indigent patients who may not be able to afford smartphones, but still, require telemedicine-guided specialist care.
To ensure efficient application of telemedicine in diabetes management, the team of endocrinologists at LAUTECH conducted a study [2] to evaluate mobile phone ownership and willingness to receive health services among diabetes patients. This survey showed that 98.3% of respondents owned mobile phones, 72.6% were willing to use phone-based diabetes services, and the most preferred mode of communication is via voice calls at 41.8%. Our report shows that mobile phones have the potential to increase access to care and reduce morbidity and mortality of diabetes mellitus patients in Nigeria.
Despite the identified barriers to telemedicine such as acceptability, infrastructure, funding, interest, the need for regulation, and concerns about patient privacy, measures can be put in place to address these challenges through teamwork and inter-faculty collaborations. An example is the recently established Department of Cybersecurity in LAUTECH which tackles information protection. Additionally, I believe that the emerging legal and ethical implications of telemedicine can be looked into by government bodies and policymakers like the Medical and Dental Council of Nigeria (MDCN).
While telemedicine cannot replace one-on-one consultation, it can go a long way to add value to traditional methods of patient care, and has often been a saving grace for many patients during the COVID-19 pandemic. My personal opinion is that physicians can be flexible in their use of telemedicine while staying cautious and pushing for necessary regulation. Many doctors are already practising telemedicine in some form but can do much more with it to advance medical practice. Hospitals should strive to incorporate telemedicine into all departments and services because it is indeed here to stay – and the earlier we embrace it, the better for our patients.
Dr Michael A. Olamoyegun is a Physician, Endocrinologist, Epidemiologist & Pharmacologist who is currently a university lecturer and a consultant physician/endocrinologist & diabetologist where he is currently the head, Department of Medicine at Ladoke Akintola University of Technology (LAUTECH) & LAUTECH Teaching Hospital (LTH) both in Ogbomoso, Oyo State, Nigeria. He is a visiting research Fellow at Hasso Platnner Institut (Digital Health), University of Potsdam, Germany.
[1] Uloko et al (Diabetes Ther. 2018 Jun; 9(3): 1307-1316
[2] Olamoyegun MA, Raimi TH, Ala OA, Fadare JO. Mobile Phone ownership and willingness to receive mHealth services among patients with diabetes mellitus in South-West, Nigeria. Pan Afr Med J.2020 Sep 8;37:29. Doi:10.11604/pamj.2020.37.29.25174.eCollection 2020.PMID:33062130.
Found this article helpful?

